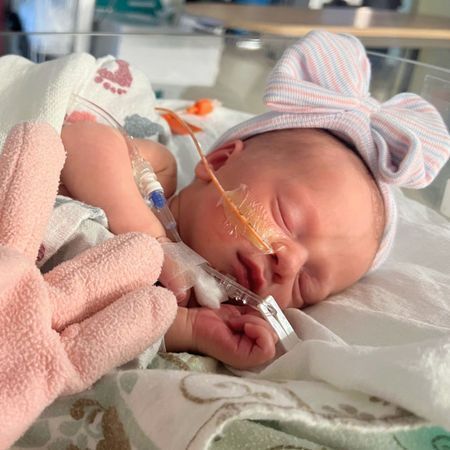
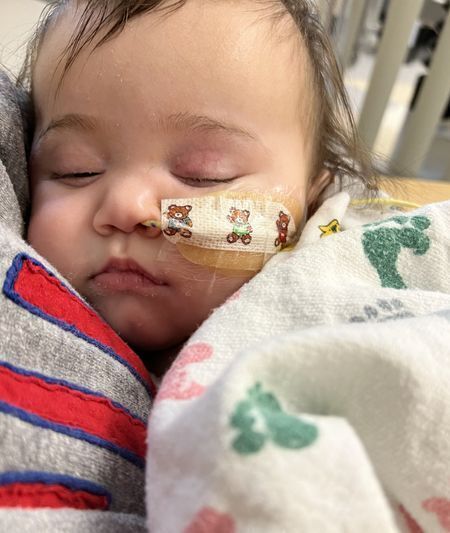
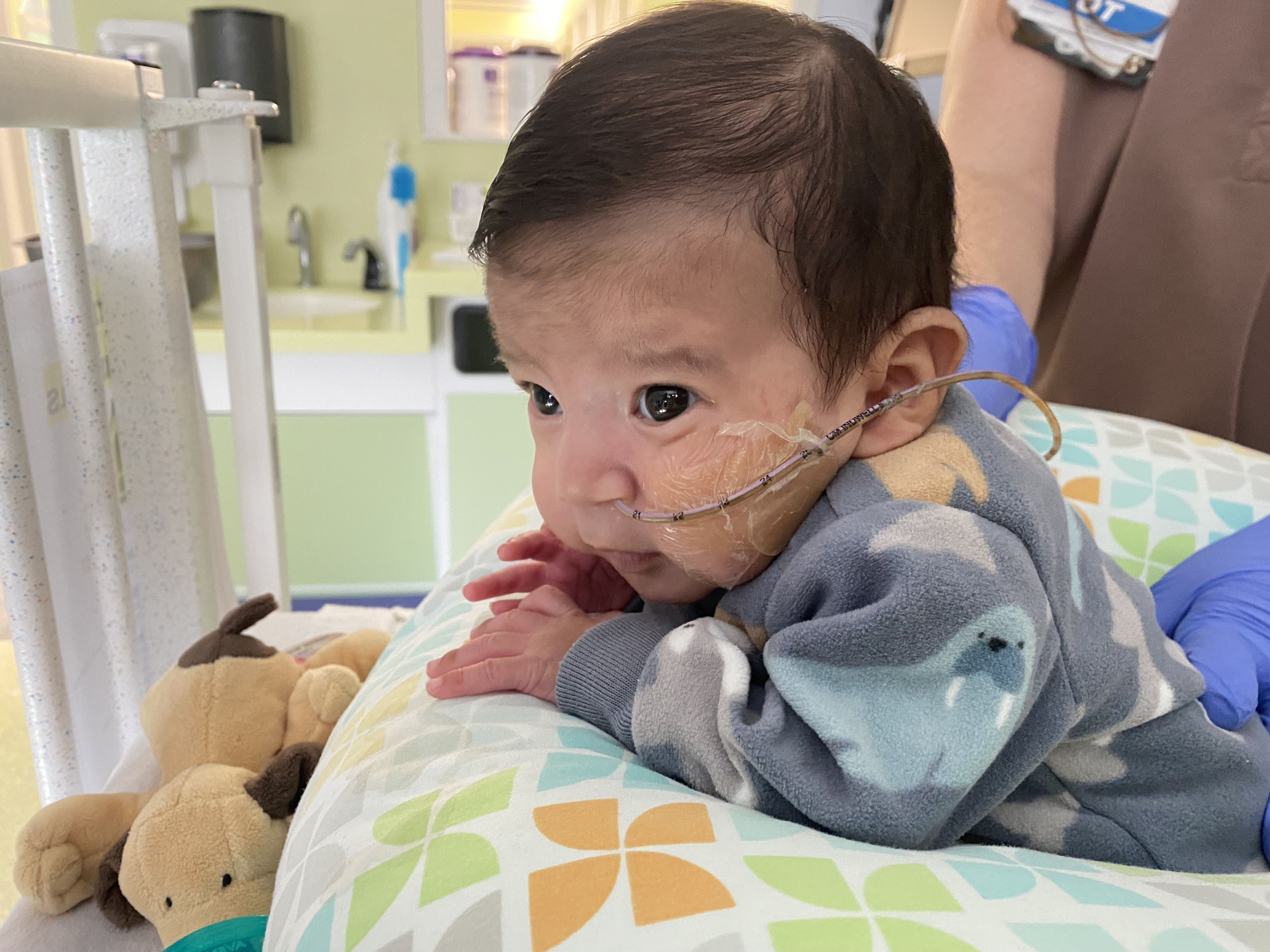
Premature Infants
- We provide fragile infants with donor milk by prescription when their own mother’s milk isn’t available. This often happens when babies are born prematurely.
- On average, 75% of donor milk is dispensed to hospital NICUs.
- Immunological properties of donor milk prevent complications such as necrotizing enterocolitis (NEC) and enhance survivability.
Outpatient Babies
- Typically, 20% of donor milk is dispensed to fragile babies at home, our outpatients.
- Outpatients with a medical necessity are never turned away based on the family's ability to pay milk processing fees.
- On average, we provide approximately $450,000 from our charitable care fund annually for these families.
Healthy Newborns
- Based on availability, approximately 5% of donor milk serves healthy newborns, bridging the gap between hospital discharge and a successful breastfeeding routine.
- Learn more about the Donor Milk To Go program.
Recipient Stories
- Read about babies who have benefited from receiving donor milk from our lab.
Breastmilk Donors
- Every year, more than a thousand mothers donate their extra breastmilk to our milk bank to help other babies. Learn about the screening process and read some of their stories.
Safety Standards
- From donor screenings to milk dispensation, we follow rigorous safety and quality assurance procedures.
Research & Education
- Review some of the research, education resources and position statements that support the utilization of donor milk for fragile infants.
Video Overview
Learn More